Calculating medical flow measurement
This column is moderated by Béla Lipták, automation and safety consultant and editor of the Instrument and Automation Engineers’ Handbook (IAEH). If you have an automation-related question for this column, write to [email protected].
Q: It was brought to my attention that in your column you might also give advice on non-industrial measurement and control topics. I have a question relating to a medical flow measurement application that involves stents. A stent is a small mesh tube that is used to keep narrow or weak arteries open. The insertion of stents is a high-risk operation and many lives could be saved, if we accurately knew if the insertion of a stent is essential or not, so that we would install a stent only in cases where blood flow is below a minimum.
If you or your colleagues have any advice or recommendation concerning this flow measurement, I and all cardiac specialists would appreciate your advice.
Z. Friedmann
[email protected]
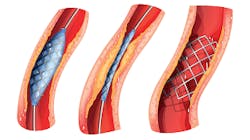
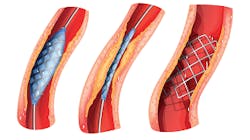
A: In this context, stents are typically mesh metal tubes that act as scaffolding, keeping the arteries pushed open (Figure 1). One non-invasive measurement method of flow is radioactive tracing. That is being used today in combination with stress tests, but they are not accurate. Some heart experts say that stents are overused for blockages that can be treated just as well with medicine, a healthy diet and exercise. One report I found indicated that some 17% of the stents inserted were not necessary and medical treatment would have sufficed.
Figure 1: Stents are inserted after the clogged vessels are cleared with a balloon to restore blood flow to the heart.
If more accurate measurements are desired than non-invasive radioactive tracing, I would recommend using optical fiber pressure sensors (OFPS), inserted in the leg and threaded up to the heart. These detectors are small (125-550 µm in diameter), immune to electromagnetic interferences, lightweight, flexible and suitable for remote monitoring.
Blood pressure is usually expressed in terms of the systolic pressure (maximum during one heart beat) over diastolic pressure (minimum in between two heart beats), and is measured in millimeters of mercury (mmHg), Resting normal systolic pressure in adults is approximately 120 mmHg and diastolic is 80 mmHg of mercury. That would be abbreviated "120/80 mmHg" and the mean arterial pressure is calculated based on these numbers.
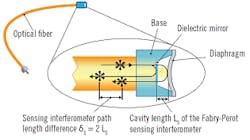
In an OFPS, the pressure modulates the intensity, phase, polarization, wavelength or transit time of light in the fiber (Figure 2).
Figure 2: Optical fiber pressure sensors (OFPS)modulate the intensity, phase, polarization, wavelength or transit time of light in the fiber.
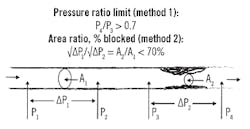
If I were designing this measurement application, I would look at it as two flow tubes (or orifices) of different cross-sectional areas (A1 and A2 in Figure 3) in series, and would use sensors to measure the pressures at four locations in the artery (P1 to P4) . Having those four readings, we can now also determine ∆P1 and ∆P2, where ∆P1 is the pressure drop through a non-restricted section of the artery and the distance between P1 and P2 is the same as the distance between P3 and P4. Once we have these measurements, we can make several calculations using methods 1 and 2, as shown in Figure 3, to determine the percentage of plugging by these different methods. It might be a good idea to make both calculations to see if their results are close to each other.
I picked the limit of 70% blockage out of the air. Conservative doctors might insert stents when the percentage of blockage is less, while others who believe that in a particular case the insertion of a stent is risky might decide to do it only if the artery is more restricted.
Figure 3: Based on four pressure measurements, one can check if the degree of blockage is high enough to justify the insertion of a stent.
Béla Lipták
[email protected]
A: This is a challenging question: The methods I would consider are:
- Sound: I suspect that you are interested in an artery deep inside the body, so that using a sensitive microphone to listen would not work.
- Ultrasound: Ultrasonic imaging might allow a look at the artery, where healthy pulsing and moving expansions might be seen and used to estimate the condition.
- Tracer: Inject an appropriate radioactive sample into the artery and use a sensor at the point of interest to detect the arrival time, the elapsed time and distance to estimate velocity, not flow. Perhaps someone else can build on this, especially the tracer method, and add to it. Any simple radiation detector could be used. Nothing fancy.
Using a tracer for flow measurement is not about the instruments, it is about the concept. This has been used to determine flows in aquifers, trace flow patterns in waste outflow, and even to discover how buried pipes are connected, and find leaks.
Cullen Langford, P.E.
[email protected]
A: I have not seen any existing instruments that do this, but I imagine that with creative thinking existing equipment could be developed. My suggestion would be to use something like the pulse measuring items, which measure heart beats, and develop a formula to adjust the heart beats to flow in particular arteries or veins.
Alex (Alejandro) Varga
[email protected]
A: My understanding is that the Nuclear stress test places a tracer in the blood and then measures the blood flow. It appears that these measurements are not accurate. Also there are a lot of blood vessels in the body. Many overlap each other, which may make measurements difficult. I had a Nuclear stress test and I passed. One day later, I had a stent placed in my LDA (known as the Widow Maker) because it was 95% blocked. That blockage was not identified by the Nuclear stress test.
Bruce Land
[email protected]